At McDermott Footcare, the first visit with a new client includes a concise assessment of pre-existing medical conditions. The reason is because pre-existing medical conditions are reflected in the health of the feet. It is important to consider what is happening to the entire body and not just the feet.
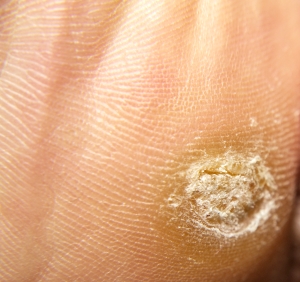
- arthritis affects the joints in the feet resulting in pain, inflammation, swelling, calluses, and corns
- a weakened immune system results in fungal and bacterial infections of the feet and toenails that are difficult to treat
- steroids such as prednisone may cause brittle, thickened toenails
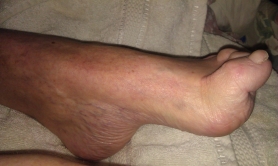
- poor circulation to the extremities from conditions such as peripheral vascular disease and diabetes may result in pain, numbness, neuropathy, swelling, changes in the colour of the skin, bacterial and fungal infections of the feet and toenails, thickening of toenails, amputation
In nursing foot care, as in all medically-related care, a wholistic approach is best. Since care at McDermott Footcare is provided by a registered nurse, counselling and health teaching is provided as needed. Clients sometimes have health-related questions and they find the knowledge and advice of a registered nurse reassuring and helpful; this gives clients peace of mind.
A wholistic approach to nursing foot care must also recognize the importance of spiritual care. Honouring the person’s spiritual dimension, irregardless of their religious beliefs, is accomplished by treating clients with respect, being nonjudgmental, and actively listening to them.
In healthcare-related professions, it is easy to focus on the procedure that must be performed, the disease that must be treated, the diagnosis that must be addressed. But the persons we care for are so much more than the diagnosis with which they present. In order to give the best care, we must always take a wholistic approach and consider each person’s mind, body, and spirit connection.
Copyright Terry McDermott. May not be reproduced in whole or in part without permission of author


You must be logged in to post a comment.